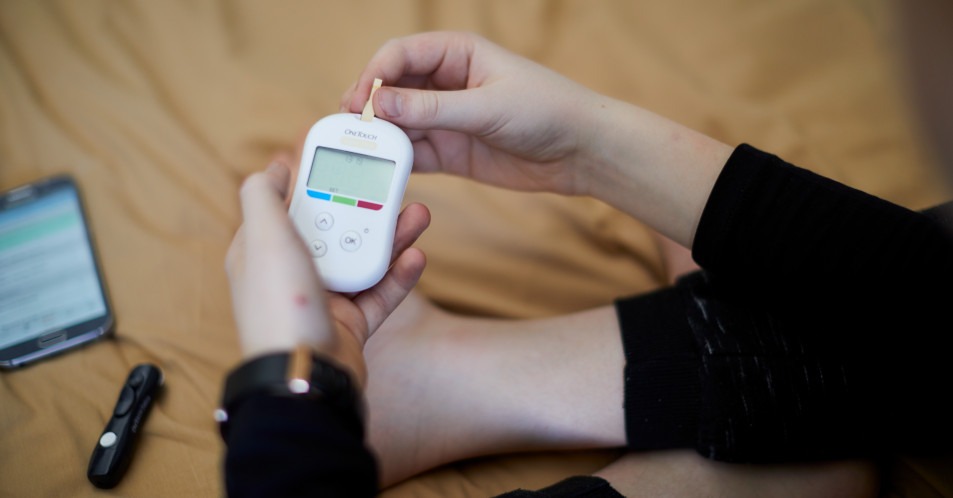
To a clinician, health care provider or even a care giver the appropriate response and actions needed in response to a Type II Diabetes diagnosis can seem clear. However, for the patient, the steps they need to take towards learning about and how to manage their new health condition can seem unmanageable. Here, we take a deeper look at what being diagnosed with Type II Diabetes can mean for a patient, the challenges they face when managing a new condition, and steps that can be taken to prevent a negative cycle of anxiety, passivity and therapy non-adherence from taking hold.
Diagnosis
A Diabetes diagnosis can be devastating. The patient is not only forced to confront the news they have a potentially debilitating chronic condition, but also that they may need to make drastic changes to often ingrained lifestyle habits or behaviors.
Understandably this reaction can lead to anxiety, often about loss of control, which also means it can be difficult to take-on the huge amount of information that clinicians share with patients following diagnosis. Patients can feel overwhelmed by their diagnosis, the amount of information they are expect to take onboard, and lack confidence in their ability to manage the condition.
In many instances – this can lead to a negative cycle of patient passivity - the opposite behavior that is required to drive successful treatment and better health outcomes.
Preventing a Negative Cycle
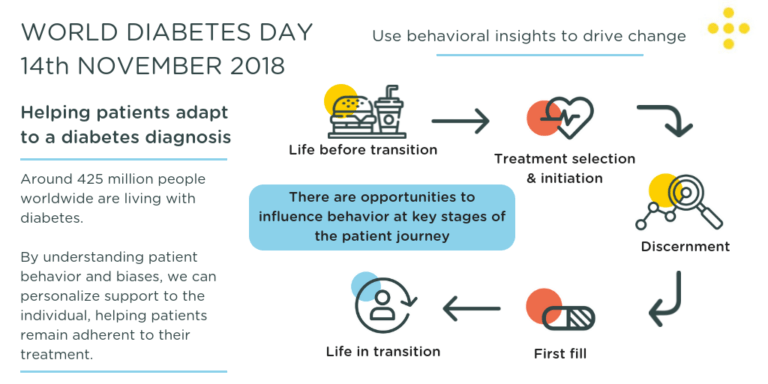 World Diabetes Day 2018
World Diabetes Day 2018
There is a need for independent, tailored support and information for patients at this stage. Information which clinicians or health care providers/HCPs feel confident in sharing in the knowledge it which help patients understand and manage their condition post-diagnosis, and that boosts the efficiency of their consultation with patients.
Once patients come to a stage of understanding about their ‘New Reality’, there is a need to support the patient as they proceed towards fulfilling their first prescription - offering the right nudges in reaction to individual concerns that may lead to a delay in starting treatment. These range from a situation where a patient has a ‘value struggle’ and can’t see what benefits the therapy will bring, to attempts to avoid or put-off starting treatment as they are potentially nervous about what it might mean for their lives - particularly with injectable therapies.
Our experience of designing tailored digital patient support programs globally has shown that an in-depth understanding of each stage of the patient journey from diagnosis onwards, and the different challenges patients may face depending on their individual circumstances is key to improving healthcare outcomes. Having this understanding enables patient support services to focus on removing the behavioral barriers to accessing and sticking with treatment.
As highlighted in one of the main themes for World Diabetes Day, it also must involve all stakeholders in the delivery of care - from Healthcare Providers, to Healthcare Professionals and family members to ensure patients with Diabetes get the support they need to understand and manage their condition, and prevent a negative cycle of patient passivity. Contact Us to find out more about our work in understanding the challenges patient face, and providing personalized support through-out their treatment journey.
Find out more about World Diabetes Day